 See also: List of radiographic findings associated with cutaneous conditionsĬT and MRI are most often used to identify intracranial abnormalities. This reduces the amount of oxygen and blood flowing to the brain, which can affect brain tissue development. In babies with SWS due to mutation of gene GNAQ, this network of nerves doesn't go away. Normally, this network goes away in the ninth week of development. Around the sixth week of development, a network of nerves develops around the area that will become a baby's head. The blood vessel formations associated with SWS start in the fetal stage. Sturge–Weber syndrome rarely affects other body organs. Increased pressure within the eye can cause the eyeball to enlarge and bulge out of its socket ( buphthalmos). Glaucoma can be expressed as leukocoria, which should suggest further evaluation for retinoblastoma. Some children will have developmental delays and cognitive delays about 50% will have glaucoma (optic neuropathy often associated with increased intraocular pressure), which can be present at birth or develop later. There may also be muscle weakness on the side of the body opposite the birthmark. Convulsions usually happen on the side of the body opposite the birthmark, and vary in severity. Neurological signs include seizures that begin in infancy and may worsen with age. This causes calcification of tissue and loss of nerve cells in the cerebral cortex. There is also malformation of blood vessels in the pia mater overlying the brain on the same side of the head as the birthmark. The birthmark can vary in color from light pink to deep purple and is caused by an overabundance of capillaries around the ophthalmic branch of the trigeminal nerve, just under the surface of the face. Sturge–Weber syndrome is usually manifested at birth by a port-wine stain on the forehead and upper eyelid of one side of the face, or the whole face. Signs and symptoms Port wine stains of an 8-year-old female with Sturge-Weber Syndrome Dilated bulbar vessels in Sturge–Weber syndrome Imaging findings may include tram track calcifications on CT, pial angiomatosis, and hemicerebral atrophy. It is caused by a mosaic, somatic activating mutation occurring in the GNAQ gene. Unlike other neurocutaneous disorders (phakomatoses), Sturge–Weber occurs sporadically (i.e., does not have a hereditary cause). Sturge–Weber is an embryonal developmental anomaly resulting from errors in mesodermal and ectodermal development. This type is only diagnosed via brain scan. The facial angioma is absent and glaucoma rarely occurs. 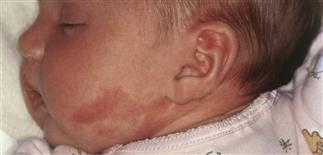
Type 3 has leptomeningeal angioma involvement exclusively. More research is needed on this type of Sturge–Weber syndrome. The symptoms can include glaucoma, cerebral blood flow abnormalities and headaches. Symptoms can show at any time beyond the initial diagnosis of the facial angioma. There is no evidence of brain involvement. Type 2 involvement includes a facial angioma (port wine stain) with a possibility of glaucoma developing. 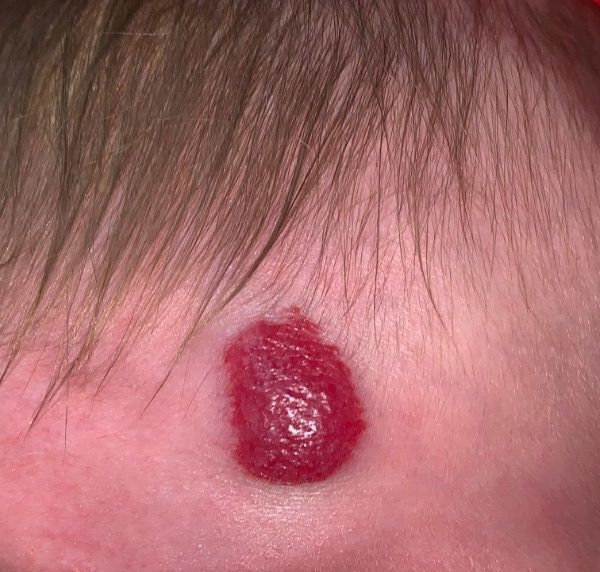
Normally, only one side of the brain is affected. Type 1 includes facial and leptomeningeal angiomas as well as the possibility of glaucoma or choroidal lesions. Sturge–Weber syndrome can be classified into three different types. It is one of the phakomatoses and is often associated with port-wine stains of the face, glaucoma, seizures, intellectual disability, and ipsilateral leptomeningeal angioma (cerebral malformations and tumors). Sturge–Weber syndrome, sometimes referred to as encephalotrigeminal angiomatosis, is a rare congenital neurological and skin disorder. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
